Resources
Our goal for this resource section is to create an all-encompassing industry resource that will include practice guidelines, useful links/handouts, and our team’s research outcomes. Check back frequently as we will continue to update this page with valuable information. Please contact us if you have any questions.
Here are links to our resource categories:
January 2018 - National Partnership to Improve Dementia Care in Nursing Homes: Late Adopter Data Report
CMS recently announced that the National Partnership met its goal of reducing the national prevalence of antipsychotic medication use in long-stay nursing home residents by 30 percent by the end of 2016. It also announced a new goal of a 15 percent reduction in those homes with currently limited reduction rates.
Nursing homes with low rates of antipsychotic medication use are encouraged to continue their efforts and maintain their success,while those with high rates of use are to work to decrease antipsychotic medication use by 15 percent for long-stay residents by the end of 2019. These homes have been identified as late adopters.
This quarterly data report is specific to the progress of the late adopters.
Click here to view the pdf data.
January 2018 - National Partnership to Improve Dementia Care in Nursing Homes: Antipsychotic Medication Use Data Report
The National Partnership to Improve Dementia Care in Nursing Homes is committed to improving the quality of care for individuals with dementia living in nursing homes. The National Partnership has a mission to deliver health care that is person-centered, comprehensive and interdisciplinary with a specific focus on protecting residents from being prescribed antipsychotic medications unless there is a valid, clinical indication and a systematic process to evaluate each individual’s need. The Centers for Medicare & Medicaid Services (CMS) promotes a multidimensional approach that includes; research, partnerships and state-based coalitions, revised surveyor guidance, training for providers and surveyors and public reporting.
CMS is tracking the progress of the National Partnership by reviewing publicly reported measures. The official measure of the Partnership is the percentage of long-stay nursing home residents who are receiving an antipsychotic medication, excluding those residents diagnosed with schizophrenia, Huntington's Disease or Tourette’s Syndrome. In 2011Q4, 23.9 percent of long-stay nursing home residents were receiving an antipsychotic medication; since then there has been a decrease of 35.4 percent to a national prevalence of 15.4 percent in 2017Q3. Success has varied by state and CMS region, with some states and regions having seen a reduction of greater than 35 percent.
Click here to view the pdf data.
A four-quarter average of this measure is posted to the Nursing Home Compare website at https://www.medicare.gov/nursinghomecompare/
ISDH Makes Survey Region Changes
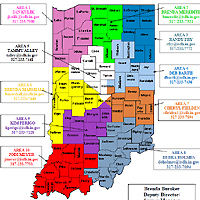
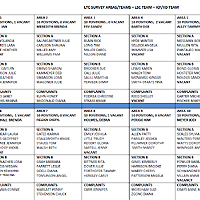
The ISDH periodically realigns its survey areas because of changes to the number of facilities in an area or changes in the location of surveyors. Long term care (LTC) survey areas will be changing effective April 1, 2015.
Click here to view pdfs of the updated Survey Area Map and LTC Survey Area Teams.
CMS Rule: Separation of consultant pharmacist from provider pharmacy
In late 2011 CMS proposed separation of consultant pharmacist from provider pharmacy:
- Rationale for separation: Reduce source(s) of conflict (Consultant Pharmacist with Provider Pharmacy with Drug Manufacturers and Rebates)
- Goal of separation: Increased quality of service, increased patient safety, decreased healthcare costs.
Click here to continue reading about the CMS Rule and the options you have.
TOP
Prevent, Recognize, Treat: Infection
"Surveillance Definitions of Infections in Long-Term Care Facilities: Revisiting the McGeer Criteria" from The Society for Healthcare Epidemiology of America. These updated definitions are intended to serve as a national standard for infection surveillance in LTCFs.
Click here to view this pdf resource.
TOP
Facts & Stats
Medications
• Each day more than 10,000 baby boomers will reach the age of 65, and this will continue daily until 2030.1
• On average, individuals 65 to 69 years old take nearly 14 medications per year while individuals aged 80 to 84 take 18 medications per year.2
• Seniors represent just over 13% of the population, but consume 40% of prescription drugs and 35% of all over-the-counter drugs.2
• 15% to 25% of drug use in seniors is considered unnecessary or otherwise inappropriate.2
Adverse Drug Reactions
• Adverse drug reactions are the 4th leading cause of death in the United States.3
• More than 200,000 people die and another 2.2 million are injured each year because of medication-related problems— and seniors are the most susceptible.4
• Adverse drug reactions increase exponentially with 4 or more medications.5
• 59% of adverse drug reactions are preventable.6
• The risk for medication problems increases with the normal aging process. Additionally, an increased sensitivity to medications often occurs.7
• 36% of all reported adverse drug reactions involve an elderly individual.2
• Adverse drug reactions and noncompliance with medications are responsible for 28% of hospitalizations in the elderly.2
• Each year 32,000 seniors suffer hip fractures caused by medication-related problems.2
Medication Adherence
• Two-thirds of all patients do not take their medications as prescribed and adherence is lowest among patients with chronic illnesses.8,9
• At least 125,000 Americans die annually due to poor medication adherence.10
• As adherence declines, emergency room visits increase by 17% and hospital stays rise 10% among patients with diabetes, asthma, or gastric acid disorder.11
Health Care Cost
• For every $1 spent on medications, $1.33 is spent on medication-related problems.12
• In the community population, medication-related problems cost $177.4 billion a year representing a 57% increase in only five years.4
• Medication problems are the cause of more than 250,000 hospital stays in people ages 65 and older each year. These hospitalizations are often avoidable and cost an estimated $20 billion.13
• Compounding the public health problem, seniors may not be taking the medications they need because they cannot afford them. Poor medication adherence results in 33% to 69% of medication-related hospital admissions in the United States, at a cost of roughly $100 billion per year.7,14
• It is estimated that total potential savings from adherence and related disease management could $290 billion annually or approximately 13% of health spending.15
• The elderly account for 42% of the $102 billion total annual drug spending in the U.S.7
• The number of seniors needing long-term care is projected to rise to 13.8 million by the year 2030 while only 5.3 million will reside in nursing homes and other long-term care facilities.16
Resources
1. Cohn D, Taylor P. Baby boomers approach 65. Available at: www.pewsocialtrends.org Accessed July 17, 2014.
2. Food and Drug Administration Report. 1996.
3. Food and Drug Administration. Preventable Adverse Drug Reactions: A Focus on Drug Interactions. Available at: www.fda.gov Accessed July 17, 2014.
4. Ernst F. R., Grizzle A. J. Drug-related morbidity and mortality: updating the cost-of-illness model. J Am Pharm Assoc. 2001;41:192–9.
5. Jacubeit T, Drisch D, Weber E. Risk factors as reflected by an intensive drug monitoring system. Agents Actions 1990;29:117–125.
6. Department of Health and Human Services. Office of the Inspector General. Adverse events in skilled nursing facilities: national incidence among medicare beneficiaries. Feb 2014.
7. Families USA. Cost overdose: growth in drug spending for the elderly, 1992-2010. Available at: research.policyarchive.org Accessed July 17, 2014.
8. Sokol MC, McGuigan KA, Verbrugge RR, Epstein RS. Impact of medication adherence on hospitalization risk and healthcare cost. Med Care. 2005; 43:521-30.
9. Greenberg QR. Survey conducted for Prescriptions for a Healthy America. May 2013; Available at adhereforhealth.org
10. McCarthy R. The price you pay for the drug not taken. Bus Health. 1998;16:27-28,30,32-33.
11. Goldman D. Pharmacy benefits and the use of drugs by the chronically ill. J. of the Amer. Med. Ass’n. 19 May 2004.
12. The American Society of Consultant Pharmacists. Medication-related problems (MRPS) in older adults: a hidden and costly epidemic. 2008.
13. Bates D. W., Spell N., Cullen D. J. et al. The costs of adverse drug events in hospitalized patients. JAMA 1997;277:307–11.
14. Osterberg L, Blaschke T. Adherence to Medicatio. New Engl. J. Med., 2005;353(5):487-497.
15. NEHI Research Brief. Thinking Outside the Pillbox: A System-wide approach to Improving Patient Medication Adherence for Chronic Disease. NEHI, 2009.
16. U.S. Department of Health and Human Services. Administration on Aging. A Profile of Older Americans. 2002.
News & Events
2015 Forum on Aging
& Annual Meeting
March 3 - 4, 2015
Council on Aging of Southwestern Ohio
2015 Spring Conference
& Trade Show
May 4-5, 2015
LeadingAge Indiana
More Details
Industry Resources

 Practice Guidelines
Practice Guidelines Research
Research Follow us on LinkedIN
Follow us on LinkedIN Follow us on Facebook
Follow us on Facebook